Medical Credentialing Services
From application to approval, we manage the entire credentialing process with accuracy and speed. Whether you’re just launching your practice or expanding into new networks, we help you get enrolled with major payers efficiently. The result? Timely and predictable reimbursements.
Credential Providers Across 75+ Specialties in All 50 States
Our customized physician credentialing services cater to a broad spectrum of healthcare professionals, such as:
- Health systems and hospitals
- Physicians (MDs and DOs)
- Nurse Practitioners (NPs) and Physician Assistants (PAs)
- Registered Nurses (RNs)
- Physical and Occupational Therapists (PTs & OTs)
- Speech-Language Pathologists (SLPs)
- Chiropractors (DCs)
- Dentists and dental specialists
- Optometrists
- Podiatrists (DPMs)
- Clinical Psychologists
- Clinical Social Workers
- Marriage and Family Therapists (MFTs)
- Specialized rehabilitation and therapy centers
- And other licensed practitioners and allied health specialists


Documentation Checklist (Essential for All Applications)
For our medical credentialing services, we will be needing the following documents from you:
- State medical license
- DEA/Controlled Substance license
- Board certifications
- Medical school diploma & residency verification
- Work history with no gaps
- Malpractice insurance and claims history
- Disclosure of sanctions/exclusions
- Curriculum Vitae
- DEA number and taxonomy details
- CAQH profile and attestation
What Makes Us the Best Medical Credentialing Company?
24/7 Status Visibility
Monitor application progress anytime with our online portal.
Faster Turnaround
Cut credentialing time down from months into weeks.
Reduced Admin Burden
Focus on patient care instead of paperwork.
Timelines You Can Count On
Below are typical timelines for our insurance credentialing services:
- Commercial Insurance Plans (e.g., Aetna, Cigna, UnitedHealthcare, BCBS)
Usually complete credentialing in 45–60 business days. - Medicare Enrollment (via PECOS & MACs)
Most Medicare enrollments close in 45–60 days.
Medicaid (State-Specific Programs)
Bring it down to 50–70 days.

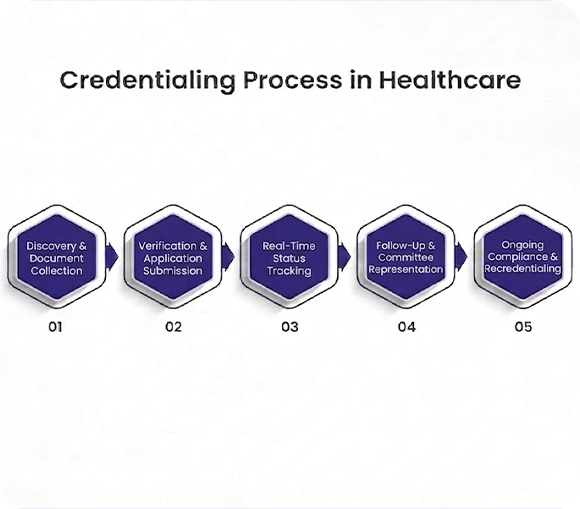
Our 5-Step Credentialing Methodology
Step 1: Discovery & Document Collection
Audit your credentials and compile a complete responsive packet.
Step 2: Verification & Application Submission
Submit to PECOS (Medicare), state Medicaid, and commercial health plans.
Step 3: Real-Time Status Tracking
Dedicated dashboard, credential coordinator assigned, and weekly updates.
Step 4: Follow-Up & Committee Representation
Manage all requests, corrections, and committee responses until final approval.
Step 5: Ongoing Compliance & Recredentialing
Automatic alerts before license or certification expiry + annual monitoring.
What We Offer
Our Core Physician Credentialing Services
- Medicare & Medicaid Enrollment
Manage Medicare enrollment using CMS-855I, CMS-855B, and CMS-855R forms. Complete state Medicaid enrollments such as Medi-Cal and TMHP, keeping billing active and preventing interruptions.
- Commercial Insurance Credentialing
Complete credentialing for UnitedHealthcare, Aetna, Cigna, Blue Cross Blue Shield, and local plans. Handle applications, document requests, and re-credentialing cycles every 2 to 3 years.
- MCR DMEPOS Enrollment
Submit the CMS-855S application for Medicare DMEPOS enrollment. Meet National Supplier Clearinghouse requirements and keep correct surety bonds for Medicare payments.
- CAQH Registration
Set up your CAQH ProView profile and upload required documents. Complete attestation every 120 days to support payer reviews for Aetna, Cigna, and Anthem.
- PECOS Management
Manage your PECOS account and keep enrollment details current. Handle changes in ownership, practice locations, and reassignment so Medicare records stay accurate.
- Revalidation Tracking
Track revalidation dates across Medicare, Medicaid, and commercial payers. Update your information in PECOS and CAQH to avoid deactivation and costly claim denials.
- NPI Registration (Type 1 & 2)
Prepare and maintain Type 1 and Type 2 NPIs through the NPPES portal. Keep identifiers accurate to support HIPAA billing compliance and reduce claim denials.
- Hospital Privileges
Handle hospital appointment and reappointment applications, typically every 2 years. Collect CVs, peer references, malpractice history, and required forms for Medical Staff Offices.
- Provider State Licenses
Manage new state license applications, renewals every 1 to 2 years, and CME tracking. Support multi-state licensing through the Interstate Medical Licensure Compact.
- DEA Registration
Assist with DEA registration and renewals every 3 years. Maintain compliance with the Controlled Substances Act to avoid delays in prescribing authority.
- Contract Negotiation
Review payer contracts for UnitedHealthcare, Aetna, Cigna, and BCBS. Negotiate better fee schedules and clearer payment terms to reduce underpayment and disputes.
- Primary Source Verification
Verify education, training, licensure, board certification, and malpractice history. Follow NCQA, URAC, and The Joint Commission standards to support approvals and audits.
Do you know your providers’ true effective dates with each payer?
Performance Snapshot
Results You Can Expect
Over the past decade, Manifest Technology Solutions has supported healthcare organizations with structured credentialing and payer enrollment services with measurable outcomes:
- 98% on-time submissions
- 35% fewer enrollment delays
- 25–40% faster network activation
- 99% documentation accuracy
- 90%+ first-pass approvals

Frequently Asked Questions
Timelines vary by payer, but most large commercial insurance companies complete credentialing and contracting within 90–120 days. Smaller or regional plans may take longer due to slower internal processes.
The process has two stages:
- Credentialing: The payer verifies licenses, education, work history, and background, then submits the file for committee approval.
- Contracting: After approval, the participation agreement is finalized and an effective network start date is assigned.
Commercial insurers do not allow retroactive billing. You may only bill for services provided after your enrollment is active in the payer’s system. Billing out-of-network can result in higher patient responsibility, including potential full self-pay balances.
DMEPOS enrollment is more involved and usually takes longer. Applications undergo enhanced review and require an on-site inspection. During the visit, inspectors verify:
- The business operates at the listed address
- Posted business hours
- Inventory storage
- Compliance with DMEPOS operational standards
Most individual providers must revalidate every five years, though certain high-risk provider types may be required to revalidate more frequently.
- Individual providers: CMS-855I (paper) or PECOS (online)
- Group practices/suppliers: CMS-855B
Once Medicare issues a revalidation request, you have 60 days to respond. Missing the deadline can result in suspended or revoked billing privileges. If EFT isn’t already on file for a group, it must be submitted during revalidation.
Requirements vary by payer and state, but most applications request the following:
Personal & Professional Documents
- CV/Resume: Full work history listed by month/year
- State professional license
- DEA certificate (if prescribing controlled substances)
- State CDS license (if applicable)
- Malpractice insurance certificate
- Government-issued photo ID
- Board certification (if applicable)
- Education or degree documentation (non-MD/DO providers)
Additional Documents (as applicable)
- Collaborative or supervising physician agreement
- ECFMG certificate (international medical graduates)
- Admitting arrangement letter
- Prescribing arrangement letter
Citizenship or immigration documents (for first-time Medicare enrollment)
Business & Entity Documents
- IRS CP575 or 147C letter (EIN verification)
- IRS W-9
- CLIA certificate (if performing lab testing)
- Office lease (often required for therapy or group practices)
- Business license
- Bank verification letter (for EFT)